دعوة للتواصل
لطالما كان الرفاه الاجتماعي جزءًا لا يتجزأ من تعريف منظمة الصحة العالمية للصحة – "“حالة من اكتمال الجوانب البدنية والعقلية و الرفاه الاجتماعي وليس مجرد غياب المرض أو العجز”ومع ذلك، ظلّ هذا الجانب مهملاً لعقود. وقد حفّزت الأدلة المتزايدة التي تربط الانقطاع الاجتماعي بأضرار جسدية ونفسية خطيرة، بما في ذلك أمراض القلب والأوعية الدموية، والسكتة الدماغية، والخرف، والاكتئاب، والوفاة المبكرة، الأبحاث والسياسات والإجراءات العملية في جميع أنحاء العالم. وقد تناولت منظمة منارة هذه المواضيع بمزيد من العمق في حوارها الصوتي الأخير؛ يمكنك مشاهدته. هنا.
لقد أبرزت جائحة كوفيد-19 هذا الأمر بشكل جليّ. فبينما سارعت الحكومات للاستجابة لما وصفه الكثيرون بـ"وباء الوحدة"، استجابت منظمة الصحة العالمية بإنشاء لجنة التواصل الاجتماعي، وهو اعتراف تاريخي بالتواصل الاجتماعي كأولوية حقيقية للصحة العامة، على قدم المساواة مع الصحة البدنية والنفسية والرفاهية. التقرير الرئيسي, يقدم التقرير المنشور في عام 2025 حجة مقنعة لاتخاذ إجراءات، ويحدد خمسة مجالات استراتيجية لتعزيز التواصل الاجتماعي على مستوى العالم، بما في ذلك القياس والتمويل وتوسيع نطاق التدخلات المثبتة والمحتملة.
فريقنا ورقة بحثية حديثة في مجلة مقاييس صحة السكان يبني على هذا الزخم المتزايد، ويساهم بأداة أساسية كانت مفقودة في هذا المجال: نظام تصنيف موحد قائم على الأدلة لتدخلات العزلة الاجتماعية والوحدة (SIL).
الابتكار بدون اتساق
مع ازدياد الوعي بالانفصال الاجتماعي، اتسع نطاق التدخلات المصممة لمعالجته. وتشمل هذه التدخلات العلاجات النفسية والسلوكية، والبرامج التي تركز على العلاقات، والخدمات الرقمية، والتغييرات في البيئات والأنظمة المادية والاجتماعية التي يعيش فيها الناس.
عند النظر في الانقطاع الاجتماعي، نجد أن جوانب مختلفة كالعزلة الاجتماعية والوحدة، رغم الخلط بينهما في كثير من الأحيان، تعمل وفق آليات مختلفة. فالعزلة الاجتماعية مقياس موضوعي لمدى تواصل الفرد فعلياً مع الآخرين، بينما الوحدة شعور شخصي بأن هذا التواصل أو العلاقات لا يلبي توقعات الفرد. وتتطلب هذه الآليات المختلفة تدخلات متباينة. ومع ذلك، فبدون لغة مشتركة لوصف هذه التدخلات وتصنيفها، تكون العواقب العملية لهذه التناقضات وخيمة.
- لا يمكن مقارنة المناهج بشكل ذي معنى من حيث الملاءمة أو الفعالية،,
- يتم تكرار الأدلة بدلاً من تجميعها.,
- يصعب تبرير أولويات السياسات والموارد،,
- لا تزال الثغرات في قاعدة الأدلة غير مرئية.
وقد أدت هذه المشكلات إلى ظهور مجموعة متنامية بسرعة ولكنها غير مترابطة من الأدلة، مما يساهم في عدم فعالية النظام والموارد وعدم كفاءتها، وهو ما ستعاني منه المجتمعات التي تواجه بالفعل قيودًا أكبر على الموارد بشكل غير متناسب.
لا يوجد حاليًا نظام تصنيف موحد لتدخلات التواصل الاجتماعي. وتُستخدم أنظمة مخصصة عند عرض المعلومات، حيث تشمل التصنيفات الأكثر شيوعًا آلية التدخل، وطريقة التنفيذ، والفئة المستهدفة. ومع ذلك، فإن غياب نظام مُعتمد سيستمر في تفاقم مشكلات الكفاءة والفعالية، مما يستلزم تطبيق سياسات ومبادئ توجيهية موحدة للممارسة.
ولمعالجة هذا الأمر، تم تطوير نظام تصنيف ASSeTS لتدخلات التواصل الاجتماعي.
الاستفادة من أصولك
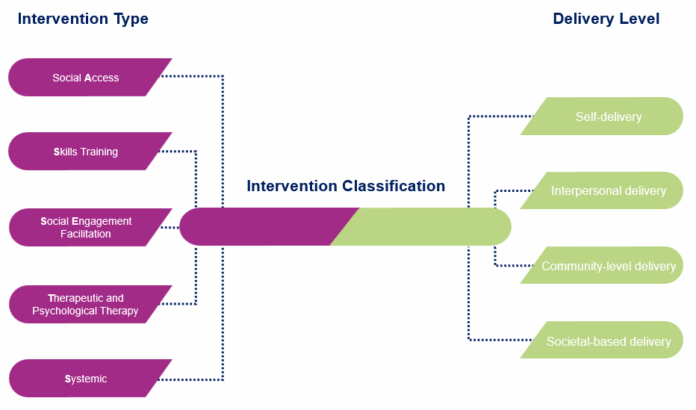
لمعالجة هذه الفجوة، تُطوّر هذه الورقة البحثية نظام تصنيف ASSeTS وتختبره تجريبيًا، وهو أول إطار عمل مُستند إلى الأدلة ومتوافق مع معايير منظمة الصحة العالمية، ومُصمّم خصيصًا لتصنيف التدخلات التي تعالج العزلة الاجتماعية والشعور بالوحدة. وقد طُوّر نظام ASSeTS من خلال مراجعة منهجية دقيقة لأنظمة التصنيف الحالية في 17 قاعدة بيانات دولية، وتمّ تحسينه عبر مشاورات متكررة مع خبراء من أعضاء المجموعة الاستشارية الفنية التابعة للجنة منظمة الصحة العالمية المعنية بالتواصل الاجتماعي. ويُحدّد نظام ASSeTS خمس فئات رئيسية من التدخلات، تشمل:
- وصول - توفير فرص للتفاعل الاجتماعي (مثل وسائل النقل الميسرة، والحدائق المجتمعية، والوصفات الاجتماعية)
- مهارات – بناء المهارات اللازمة لبناء العلاقات والحفاظ عليها (مثل التدريب على المهارات الاجتماعية، وبرامج محو الأمية الرقمية)
- المشاركة الاجتماعية – توفير تفاعلات متسقة أو منتظمة (مثل مجموعات دعم الأقران، والصداقة، والعلاج بمساعدة الحيوانات)
- العلاج النفسي والعلاجي – معالجة الحواجز المعرفية والعاطفية (مثل العلاج السلوكي المعرفي، واليقظة الذهنية)
- نظامي – التدخلات التي تؤثر على المحددات الأولية على مستوى المجتمع للانفصال الاجتماعي (مثل السياسات الوطنية، وحملات التوعية العامة، وتمويل البحوث)
يُستخدم كل نوع من أنواع التدخل جنبًا إلى جنب مع مستويات التنفيذ الاجتماعية والبيئية (التنفيذ الذاتي، والتفاعلي، والمجتمعي، والمجتمعي العام)، وذلك لاستيعاب التنوع الكامل لكيفية عمل التدخلات في الواقع العملي. على سبيل المثال، يُقارن تدخل الوصول الاجتماعي (التنفيذ الذاتي)، مثل منصات مكالمات الفيديو، بتدخل الوصول الاجتماعي (التنفيذ المجتمعي)، مثل توفير مساحات مشتركة في حي محلي. إن إدراج كل من نوع التدخل ومستوى التنفيذ الاجتماعي والبيئي يُبرز بشكل أكبر التنوع في تدخلات التواصل الاجتماعي، مما يستدعي الحاجة إلى نهج أكثر توحيدًا للتصنيف.
مع استمرار تأثير التواصل الاجتماعي على سياسات وممارسات الصحة في جميع أنحاء العالم، يُرسي مشروع ASSeTS بنيةً أساسيةً لهذا المجال. فمن خلال توفير إطار عمل موحد ومعياري، يُتيح للباحثين والأطباء وصناع السياسات أداةً لاتخاذ قرارات أكثر وضوحًا لمواجهة تحديات الصحة العالمية المعاصرة والمتطورة. ورغم الحاجة إلى مزيد من العمل لتطوير هذا الإطار مع تطور المجال، يُمثل مشروع ASSeTS خطوةً استراتيجيةً نحو تنسيق عالمي أفضل وعمل أكثر فعالية لتعزيز التواصل الاجتماعي.
ماذا يعني هذا بالنسبة لمنطقة الشرق الأوسط وشمال أفريقيا؟
في الشرق الأوسط وشمال إفريقيا، تُعد أهمية التواصل الاجتماعي كبيرة وغالبًا ما يتم التقليل من شأنها، ويوفر برنامج ASSeTS أدوات هناك حاجة ماسة إليها.
يقدم تقرير لجنة منظمة الصحة العالمية بيانات تبعث على القلق. إذ تُسجل منطقة شرق المتوسط، التي تضم جزءًا كبيرًا من منطقة الشرق الأوسط وشمال أفريقيا، ثاني أعلى معدل انتشار مُقدّر للشعور بالوحدة على مستوى العالم، حيث يبلغ 21.01 حالة لكل 3000 نسمة، ولا تتجاوزها في ذلك سوى منطقة أفريقيا جنوب الصحراء الكبرى (24.31 حالة لكل 3000 نسمة). أما بالنسبة لكبار السن، فالوضع أكثر وضوحًا: تشير البيانات المتاحة إلى أن العزلة الاجتماعية بين كبار السن في منطقة شرق المتوسط قد تكون الأعلى بين جميع المناطق، حيث تصل التقديرات إلى 46.11 حالة لكل 3000 نسمة، على الرغم من أن قاعدة الأدلة لا تزال محدودة وتستند بشكل رئيسي إلى لبنان. وفي جميع أنحاء المنطقة، نُسبت حوالي 76,500 حالة وفاة إلى الشعور بالوحدة بين عامي 2014 و2019، وهو رقم يُرجح أنه أقل من الواقع نظرًا لقلة البيانات.
تتعقد الصورة بفعل الثقافة. يشير تقرير منظمة الصحة العالمية إلى أن المجتمعات الجماعية، التي تشمل جزءًا كبيرًا من العالم العربي، غالبًا ما تسجل معدلات أقل من الشعور بالوحدة مقارنةً بالمجتمعات الفردية. ومع ذلك، لا يعود ذلك إلى قلة شيوع هذه التجربة، بل إلى كونها أكثر وصمًا اجتماعيًا. ففي السياقات التي تُعتبر فيها الروابط الأسرية والاجتماعية قيمًا راسخة، قد يحمل الاعتراف بالشعور بالوحدة أو العزلة دلالات خاصة. عار. وهذا يعني أن البيانات المبلغ عنها ذاتيًا بشأن الشعور بالوحدة في منطقة الشرق الأوسط وشمال إفريقيا من المرجح أن تقلل من شأن المدى الحقيقي للمشكلة، وأن التدخلات التي تتمحور حول أوجه القصور النفسية الفردية قد لا تلقى قبولًا جيدًا أو تكون غير متوافقة ثقافيًا.
تتداخل هذه التحديات مع التغيرات الديموغرافية السريعة. تشهد منطقة الشرق الأوسط وشمال أفريقيا شيخوخة سكانية أسرع من أي منطقة أخرى في العالم تقريباً، كما أوضحت مينارا في تقريرها الأخير. الكلمة الرئيسية في مؤتمر الجمعية البريطانية لعلم النفس الاجتماعي. إن وتيرة التغير الديموغرافي في منطقة الشرق الأوسط وشمال أفريقيا غير مسبوقة. فمع التوسع الحضري والهجرة وتغير هياكل الأسرة وانتشار التقنيات الرقمية التي تعيد تشكيل الحياة الاجتماعية، لم يعد بالإمكان اعتبار الشبكات التقليدية الواقية التي كانت تحمي من الانقطاع الاجتماعي أمراً مفروغاً منه. وتتعرض النساء الأكبر سناً بشكل خاص لهذا التآكل في الشبكات الواقية، كما هو الحال في منظمة مينارا. عمل أظهرت الدراسات المتعلقة بإساءة معاملة كبار السن في المنطقة العربية أن العزلة والتبعية وفقدان القدرة على التأثير الاجتماعي تتفاقم بشكل كبير بالنسبة للنساء اللواتي فقدن أزواجهن أو اللواتي يعانين من محدودية الحركة.
تُظهر دول مثل مصر والمغرب والأردن والكويت ولبنان اتجاهات مستقرة عمومًا فيما يتعلق بالوحدة في البيانات المتاحة، بينما تُظهر الإمارات العربية المتحدة اتجاهًا تنازليًا. ومع ذلك، يجب تفسير هذه الأنماط بحذر، نظرًا للقيود الشديدة في جودة البيانات وتغطيتها. كما هو الحال في بيانات منارة الخاصة. تقرير منظمة الصحة العالمية وبالنظر إلى الاحتياجات غير الملباة في المنطقة، فإن صورة البيانات غير مكتملة بشكل كبير.
هنا تحديدًا تبرز أهمية أداة ASSeTS. ففي منطقة الشرق الأوسط وشمال أفريقيا، توجد مجموعة واسعة من مبادرات التواصل الاجتماعي قيد التنفيذ، بدءًا من الشبكات الدينية والمجتمعية المحلية، مرورًا بالمنصات الرقمية للتواصل بين المغتربين، وصولًا إلى برامج الحماية الاجتماعية الحكومية، إلا أن البحوث المنهجية التي ترصد هذه المبادرات وتقارن بينها وتقيّمها قليلة جدًا. ويُعدّ غياب إطار تصنيفي مشترك أحد أسباب عدم تراكم الأدلة حتى الآن، ولماذا تُتخذ قرارات الاستثمار غالبًا دون قاعدة بيانات واضحة.
من خلال اعتماد نظام ASSeTS، سيصبح الباحثون وصناع السياسات في جميع أنحاء المنطقة في وضع أفضل للقيام بما يلي:
- تحديد أنواع التدخلات الموجودة، أو الغائبة، أو التي لا تحظى باستثمار كافٍ في سياقات منطقة الشرق الأوسط وشمال أفريقيا.,
- بناء مجموعة تراكمية وقابلة للمقارنة من الأدلة حول ما ينجح في مختلف البيئات،,
- تصميم تعديلات متجذرة ثقافياً، لا سيما في فئتي المشاركة النظامية والاجتماعية، حيث تكون آليات المجتمع المحلي والمجتمع ككل هي الأكثر صلة بالنسيج الاجتماعي للمنطقة، و
- التفاعل مع أطر السياسات العالمية المتعلقة بالتواصل الاجتماعي من موقع الظهور الإقليمي والدعوة القائمة على البيانات.
تُشدد لجنة منظمة الصحة العالمية صراحةً على الحاجة إلى بيانات إقليمية أفضل، والتحقق من صحة أدوات القياس عبر الثقافات، وتطوير تدخلات تستند إلى سياقات ثقافية متنوعة. وتتمتع شبكة ميناراه بموقعٍ مثالي لمواجهة هذا التحدي، إذ تُسهم بأبحاث خاصة بمنطقة الشرق الأوسط وشمال أفريقيا تُغذي قاعدة الأدلة العالمية، مع ضمان أن تعكس التدخلات التي تُطور وتُختبر في المنطقة واقعها الاجتماعي، بما في ذلك الدور المحوري للأسرة والدين والمجتمع والروابط بين الأجيال في تجربة الناس للتواصل والانتماء.
نظرة مستقبلية
يُعدّ نظام ASSeTS خطوة أولى، وليس حلاً نهائياً. فهو يحتاج إلى تحسين مستمر، لا سيما في فئتي الوصول الاجتماعي والنظامي حيث كانت موثوقية التقييم بين المُقيّمين أقل، وإلى مزيد من التحقق عبر الثقافات مع تطور المجال. وينتهي البحث الأدبي الذي استندت إليه المراجعة المنهجية في سبتمبر 2023، ما يعني أن النظام سيحتاج إلى تحديث مع ظهور أدلة جديدة.
ومع ذلك، فإن الاتجاه واضح. فقد بات التواصل الاجتماعي الآن ركيزة أساسية على أجندة الصحة العامة العالمية، حيث اعتمدت جمعية الصحة العالمية أول قرار لها على الإطلاق بشأن هذه القضية في مايو 2025. وبدأت تتشكل الأدوات اللازمة لبناء استجابة أكثر تنسيقًا واستنادًا إلى الأدلة وإنصافًا. أما بالنسبة لمنطقة الشرق الأوسط وشمال أفريقيا، حيث الحاجة ماسة، والبيانات شحيحة، والسياق الثقافي يتطلب تكيفًا مدروسًا، فقد حان الوقت للانخراط.
يستند هذا إلى برنامج البحث الحالي التابع لمؤسسة مينارا، والذي يعمل باستمرار على بناء قاعدة الأدلة الإقليمية حول الشيخوخة والرفاهية – من خلال تحليل ديموغرافي للبنك الدولي, ، إلى خاصتنا تقرير منظمة الصحة العالمية حول الاحتياجات غير الملباة في مجال الرعاية الصحية والاجتماعية في شرق المتوسط, وإلى العمل الجاري حول الحقائق المعقدة للشيخوخة في منطقة الشرق الأوسط وشمال أفريقيا. يوفر مشروع ASSeTS لهذه المجموعة من الأعمال أداة جديدة: إطار عمل مشترك لطرح السؤال ليس فقط "كم عدد الأشخاص الذين يتقدمون في السن؟" ولكن "ما هي التدخلات التي تصل إليهم، وكيف، وما هي الأدلة التي تدعمها؟"“
يرجى ذكر المرجع البحثي:
سوركاليم دي إل، فرزانة أ، تشو دبليو واي، حسين إس، هيبيرت بي سي، ويلش في، تانجونغ غوغومو إي، وميكتون سي (2026). ASSeTS: مراجعة منهجية وتطوير لنظام تصنيف منظمة الصحة العالمية لتدخلات العزلة الاجتماعية والوحدة. مقاييس صحة السكان. https://doi.org/10.1186/s12963-026-00472-7

دانيال سوركاي
الدكتور دانيال سوركاليم زميل في كلية الطب والصحة بجامعة سيدني، أستراليا. شغل دانيال سابقًا منصب الخبير الصحي والفني في لجنة التواصل الاجتماعي التابعة لمنظمة الصحة العالمية، حيث ساهم في تأسيس اللجنة وإعداد التقرير العالمي لمنظمة الصحة العالمية حول التواصل الاجتماعي. يركز عمله على دراسة العلاقة بين الصحة الاجتماعية والرفاه وعلم الأوبئة، وقد نشر أكبر دراسة عالمية حول انتشار الشعور بالوحدة، كما ساهم في تطوير نظام تصنيف منظمة الصحة العالمية لتدخلات التواصل الاجتماعي. تشمل مجالات خبرة دانيال الأخرى الوقاية من الأمراض وتعزيز الصحة، والاستدامة، وتطوير الأطر.