We are living through two of the most significant transformations in modern history simultaneously: rapid population ageing and accelerating climate change. Separately, each presents enormous challenges for health and care systems. Together, they represent something far more urgent, and far less recognised in policy circles than it should be.
A paper I recently published in the journal Sustainability sets out to address this gap directly. Drawing on a horizon-scanning review of evidence from across high-income countries, the paper proposes a new framework that, for the first time, systematically integrates climate risk and adaptation into the architecture of long-term care (LTC) systems. For members of the MENARAH network, the implications are immediate and pressing.
The problem no one is planning for
Long-term care systems support older adults and people with disabilities who need sustained help with daily life, whether at home, in residential facilities, or through community services. These systems depend on stable infrastructure, a reliable workforce, functioning supply chains, and consistent funding. What the evidence makes clear is that climate hazards threaten every single one of these foundations.
Heatwaves increase hospitalisation and cognitive decline among older adults. Floods drive up care dependency among survivors. Wildfires force mass evacuations of residents who cannot move without assistance. Air pollution accelerates dementia. Power outages disrupt medical devices, medication storage, and indoor temperature control in care homes. And in each of these scenarios, it is the most vulnerable, those already living with disability, dementia, chronic illness, or social isolation, who bear the greatest burden.
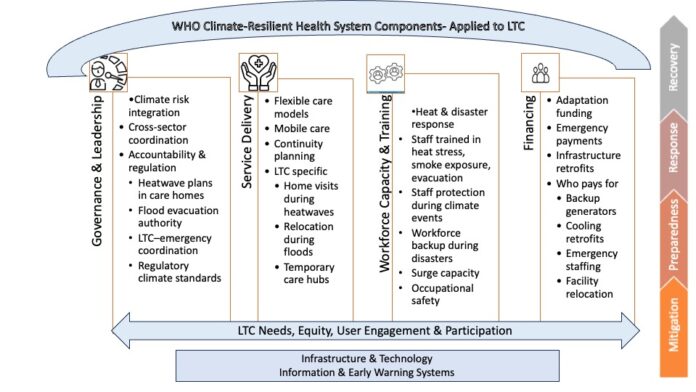
What makes this particularly troubling is not just the scale of the risk, but the policy blind spot that surrounds it. The World Health Organisation has developed two important frameworks: one for climate-resilient health systems and one for integrated long-term care. Neither references the other. Long-term care does not appear in climate adaptation strategies. Climate risk does not appear in care planning. The result is a sector left entirely at the margins of both agendas.
A framework to bridge the gap
The paper responds to this gap by proposing a climate-tailored integrated LTC framework, one that brings these two WHO frameworks into dialogue and operationalises climate resilience specifically for care systems. It is structured around four core domains: the care needs of LTC users, governance, service delivery, and system enablers (with a particular focus on workforce and financing). Cutting across all four domains are three principles that cannot be treated as add-ons: equity, user participation, and decarbonisation.
The framework recognises that physical, institutional, and social infrastructures form the foundation of any resilient care system. Physical infrastructure, such as buildings, energy, water, and transport, is directly exposed to climate hazards. Institutional infrastructure, including governance arrangements, regulations, and workforce systems, determines how well a system can prepare and respond. And social infrastructure, the community networks, informal caregivers, and peer support that hold so many care arrangements together, is what sustains people during and after climate shocks.
The framework also takes seriously what is sometimes called the climate-brain health nexus: the growing evidence that heat exposure, air pollution, and social disruption caused by climate events accelerate cognitive decline and increase dementia risk. This matters not only for individuals, but for the systems trying to care for them. As climate change intensifies, demand for long-term care will rise at the same time as the systems providing that care face greater disruption.
Why this matters for the MENA region
The evidence base drawn upon in this paper comes primarily from high-income countries, and I want to be transparent about that limitation. But the vulnerabilities and mechanisms it identifies, infrastructure dependence, workforce fragility, care continuity risks, and the compounding effects of poverty and social isolation, are not confined to any single national model. In many ways, they are more acute in contexts where formal care systems are still developing, family-based care is already under strain, and climate exposure is among the highest in the world.
The MENA region faces some of the most severe climate hazards on earth. Extreme heat, prolonged drought, dust storms, and flooding are not future projections for much of this region; they are present realities. At the same time, populations across MENA are ageing at a historically unprecedented speed. Countries that high-income nations had decades to adjust to are taking place over a single generation. And the care systems that older people will depend on, whether formal services or family networks, are already under enormous pressure.
What this means in practice is that the MENA region urgently needs to begin integrating climate risk into care planning now, before systems are overwhelmed, before a major climate event exposes the fragility of existing arrangements, and before the window for anticipatory action closes.
What needs to happen
The framework I propose is not a blueprint for a single country. It is a policy-oriented architecture that can be adapted to different institutional capacities, resource contexts, and hazard profiles. But there are some immediate priorities that apply broadly.
Governments and local authorities need to begin integrating climate risk assessment into how care services are regulated and planned. Care providers need continuity plans that account for multi-hazard scenarios, not just a single emergency. Workforce protection, retention, and climate-informed training must be treated as central to system resilience, not optional extras. And financing mechanisms need to begin aligning with national climate adaptation strategies, so that care systems are not always the last sector to receive attention and resources.
Above all, equity must be at the centre of every decision. Climate hazards do not affect everyone equally. Older adults who are poor, isolated, living with disability, or in substandard housing face compounding layers of vulnerability. Any adaptation strategy that does not explicitly address these inequalities will simply entrench them.
An invitation to engage
This paper is one step in what I hope will be a much larger conversation, one that the MENARAH network is uniquely placed to contribute to. The region’s experience of climate extremes, combined with its rich traditions of family care and community solidarity, offers perspectives that the global literature has largely overlooked.
I would welcome your reflections, your experiences, and your challenges. The evidence from MENA is urgently needed, and your voices matter in shaping how the world responds to this intersection of ageing and climate change.
The full paper is open access.
Founder and Director
Shereen Husseinis a Health and Social Care Policy professor at the London School of Hygiene and Tropical Medicine (LSHTM), United Kingdom.
Shereen Founded the MENARAH Network in 2019, through an initial grant from the Global Challenge Research Fund, UKRI. She is a medical demographer with expertise in ageing, family dynamics, migration and long-term care systems. Shereen regularly collaborates with the United Nations, the World Health Organisation and the World Bank in policy and research focused on ageing in the Middle East and North Africa Region.
Shereen received her undergraduate degree in statistics and a postgraduate degree in computer science at Cairo University. She completed an MSc in medical demography at the London School of Hygiene and a PhD in quantitative demography and population studies at the London School of Economics and Political Science, United Kingdom.